Calving Management
Care for Calf
Neonatal Calf Care
Breathing

Calf stimulation
Tickling the calf's nostril with a piece of straw or hay can
stimulate the calf to sneeze or breathe.
Image credit: Grant Dewell

Oxygen supplementation
Some calves may benefit from oxygen supplementation.
Image credit: Grant Dewell
Once the calf has been delivered spend some time making sure that the calf is adjusting to life outside the womb. The first thing a newborn calf has to do is breath. During the birthing process the umbilical cord was severed and the calf now needs to breath in order to supply oxygen to its cells. A calf that was born from a dystocia event may have fluid in its nasal passages. Remove any fetal tissues or mucus from the calf's nose and mouth. Tickling the calf’s nostril with a piece of straw or hay can stimulate the calf to sneeze and clear the nasal passages.
Practices such as hanging the calf upside down or swinging the calf are not beneficial and can actually hurt the calf or make it harder for it to breath. Fluid from the birth process is generally not in the calf’s lungs. If you do hang a calf upside down or swing it, any fluid you note coming from the calf is likely from its digestive tract. The fluid in the animal’s digestive tract can be beneficial for both hydration and nutrition and practices that remove it should be avoided. In addition, hanging the calf upside down or swinging the calf can make it harder for the calf to breath because this creates a situation where the abdominal contents put pressure on the thorax. This pressure on the thorax makes it harder for the calf to expand its lungs and breathe properly.

Hanging calf upside down
Practices such as hanging the calf upside down or swinging the calf are
not beneficial and can actually hurt the calf or make it harder for it to
breathe.
Image credit: Andrew Kingsbury
In severe cases, aspirating fluid from the nasal passages and back of throat can be accomplished with a bulb syringe. Other methods to stimulate breathing or sneezing are tickling the calf’s nasal passages with a piece of straw, wiggling a finger in calf’s ear briefly, and pouring cold water in ear canal or over the head can stimulate a gasp reflex. Pinching the nasal septum (the area between the nostrils) also can stimulate a breathing reflex. Once the calf’s nasal passages have been cleared and breathing stimulated, prop the calf in sternal recumbency (breast bone on ground, back legs under calf and front legs out front with head resting on legs) to allow easier lung function.
Calves that have problems breathing can be supplemented with oxygen to ease their adjustment. A small oxygen bottle, regulator, and tubes that are portable to easily move around can be purchased online or from a medical supply store. Ideally the oxygen flow should be regulated to flow about 5 liters per minute. The oxygen can be delivered by a small flexible tube that can be taped into the nose or a mask that covers the nose and mouth can be used. The mask can either be a special mask made for calves or a plastic bottle can be used. If you don’t have a medical oxygen tank to dedicate to your calves, you can use oxygen from an oxygen/acetylene torch if available (just make sure the acetylene is turned off.) Have the oxygen flow at a rate that feels like a gentle breeze against your face.
For calves with extreme difficulty breathing, ventilation may be beneficial. There are several commercial calf resuscitators available that have a mask and some sort of device that will push air into the lungs. Some devices utilize a tube that is inserted into the trachea to increase the efficiency of ventilating the lungs.
Checking for Heartbeat
Once the calf is breathing properly check for a heartbeat. If the heart is not beating you can attempt external cardiac massage. Gentle intermittent compressions (about one compression every second) with your palm over the cardiac area (the area underneath point of elbow) may be beneficial to revive the calf.
Drying Calf
Once the calf is breathing and heart is beating, properly dry the calf briefly. Rubbing the chest and back with a towel stimulates the calf as well as begins the drying process.

Equipment
Equipment for oxygen supplementation may be advantageous to
purchase for some producers.
Image credit: Grant Dewell
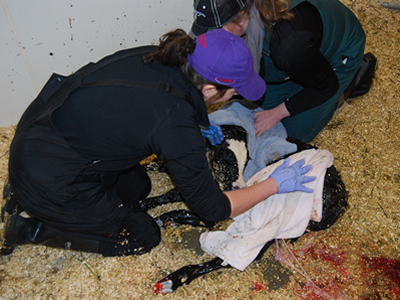
Towel rubbing
Rubbing the calf with towels helps to dry the calf as well as stimulate it.
Image credit: Grant Dewell
Ideally, place the calf in a bed of straw that can be placed in front of the cow while she is still locked in the head gate. This will keep the calf comfortable while the cow begins licking the calf dry and initiating the beginning of calf bonding.
Provision of Nutrition
While the cow is licking the calf, milk out 1 to 2 pints of colostrum for the calf. Dystocia calves are expected to have some loss of vigor and may not stand and nurse right away. Tubing the calf with colostrum prior to putting into a pen with the cow will assure that passive transfer of antibodies to the calf initiates correctly if the calf won’t nurse from a bottle. To test whether a calf is likely to nurse from a bottle, place your finger in the calf’s mouth. If the calf doesn’t suckle, then its suckle reflex may not be strong enough to consume a bottle and tube feeding should be considered. Once tubed or bottle-fed, if the calf has not stood on its own and nursed more colostrum within 4 hours, then additional colostrum should be obtained and administered to the calf. Six to ten percent of the calf’s weight should be consumed within the first 12 hours of life.
Compromised Calves
Warming Calves
Calves born with reduced vigor due to dystocia or other causes are often not able to maintain body temperature in cold environments. Additionally, even normal calves born into a wet, cold environment may not be able to maintain normal body temperature. Calves can die from hypothermia shortly after birth in severe cases. Neonatal calves do not have body reserves to maintain body temperature long term. Calves rely on energy intake from colostrum in the first 24 hours of life.

Placement in front of cow
Placing the calf in front of the cow lets the cow and calf begin to bond
and provides an opportunity for the cow to lick the calf to dry it and
stimulate it.
Image credit: Grant Dewell
Recognition of cold calves is not always immediately obvious. For example, not all cold calves will shiver. Some signs of cold calves that need intervention may include a cold nose, cold and pale hooves, failure to rise and nurse, and marked clumsiness. A thermometer is the most reliable tool to identify cold calves. Immediately following birth, a normal calf will have a temperature of about 103℉ and it should fall to 101.5°F-102°F. Interventions to warm calves should be considered for calves that are less than 100 degrees Fahrenheit. Chilled calves should be warmed up as soon as possible as the window of opportunity to warm them up is approximately 4-6 hours. Immersion in warm water (100°F) has been shown to be the most effective method of rewarming chilled calves. However, it can be difficult and labor intensive to keep calf from drowning. Generally immersion requires using the family bathtub as most operations don’t have facilities in barn to maintain an immersion warming system. Calves that are mildly chilled can be warmed by drying off the calf with towels, hair dryers, or space heaters, and placing in a warm environment. Be careful not to rub the calf too hard with towels as very cold calves sometimes have tissue damage that can be exacerbated by very vigorous rubbing. Severely cold stressed calves may need more aggressive warming scenarios. Hot boxes, either purchased or homemade ![]() , can be a suitable method to warm hypothermic calves. When the calf in a hot box breathes warm air, it helps increase core body temperature because the blood passes through the lungs where it is exposed to the warm air being breathed in by the calf. Problems with hot boxes can be extreme heat, disease transmission if boxes are not kept clean, and lack of air flow. Temperature inside a hot box should not exceed 105°F. Once calf has started to warm up, tubing with warm colostrum for new born calves or warm milk replacer for older calves will help the calf maintain temperature.
, can be a suitable method to warm hypothermic calves. When the calf in a hot box breathes warm air, it helps increase core body temperature because the blood passes through the lungs where it is exposed to the warm air being breathed in by the calf. Problems with hot boxes can be extreme heat, disease transmission if boxes are not kept clean, and lack of air flow. Temperature inside a hot box should not exceed 105°F. Once calf has started to warm up, tubing with warm colostrum for new born calves or warm milk replacer for older calves will help the calf maintain temperature.
Colostrum
A calf is born without a functional immune system and relies on the passive transfer of antibodies from colostrum for immune function for the first 3 months of life. Adequate colostral intake in the first 12 hours has a lifelong effect on the health and productivity of the calf. Improved performance and health of steers and heifers that have received adequate colostral intake has been demonstrated through the feedlot or development phase. Intake of adequate colostrum within 12 hours after birth is key to having a healthy calf. Although the calf may be able to absorb immunoglobulins from colostrum for up to 24 hours, their ability to absorb colostrum decreases linearly from birth to 24 hours. Therefore at 12 hours their ability to absorb immunoglobulins has decreased by about 50%. Any colostrum they absorb after 12 hours is still beneficial but they will be unable to obtain optimal absorption if colostral intake is delayed until 12 hours after birth.

Bottle or feeder
Delivery of colostrum using a bottle or esophageal feeder helps
provide important nutrients to calves, particularly dystocia calves.
Image credit: Grant Dewell
For the neonatal calf, adequate colostral intake is critical for proper health. Calves that do not receive enough colostrum are more likely to become sick and or die from calf diarrhea or pneumonia. Beef calves need at least 2 quarts of colostrum in the first 12 hours of life. If the calf is able to nurse its dam then 1 to 2 pints is sufficient to get the calf started. However, if the calf will be bottle raised or grafted onto another cow, it will need to be supplemented with at least 2 quarts of colostrum spread out over 3 to 4 feedings in the first 12 hours after birth.
Generally, the colostrum from the calf’s dam should be adequate to protect the calf. However, cows in poor body condition will not have the quantity and quality of colostrum that a cow in good body condition will. Also, heifers will produce less colostrum that may not have as many antibodies in it as mature cows will. As risk factors for lack of transfer increase (age and body condition of dam, dystocia events, cold or muddy conditions, poor mother) the need to supplement colostrum increases. The best sources of colostrum in decreasing order are: calf’s dam, another beef cow in herd, beef cow from another herd, dairy colostrum, and commercial colostrum replacer.
Storing Colostrum
The best source of colostrum is from your own cows. Cows that deliver a stillborn calf or have a calf die shortly after birth should be milked out and the colostrum saved for future use. Since beef cattle colostrum is more concentrated than dairy colostrum smaller amounts are needed. Fresh colostrum can be stored in the refrigerator (33-35°F) for up to seven days. One quart of beef colostrum can be frozen for up to a year in a 1-gallon zipper freezer bag. If possible, avoid the use of “frost free” freezers because the freeze-thaw cycles may damage the colostral antibodies. One quart of colostrum frozen flat in a 1-gallon bag will defrost rapidly in warm water when needed.
Care must be taken to thaw appropriately as excessive heat, uneven heating, freeze/thaw cycles, etc. can damage antibodies in colostrum. The best method for thawing 1-quart bags or containers is to place the frozen bag or container in a warm water bath (110°F) and stir every five minutes, continuing until the colostrum reaches 104°F. This thawing process takes approximately 40 minutes.
Supplemental Sources of Colostrum
Beef producers are sometimes interested in obtaining frozen colostrum from dairy operations which regularly freeze and store colostrum. When considering this option it is important to remember two potential issues. First, colostrum from dairy cows is much less concentrated than that of beef cows so it will require a greater volume to impart the same immunity if using dairy-derived colostrum. Additionally, several infectious diseases are more prevalent in dairies than in beef operations and when using dairy-derived colostrum, biosecurity has to be a concern. At a minimum, you should be confident that all stored/frozen colostrum is free of blood, mastitis organisms, Johne’s disease, bovine leukemia virus and fecal contamination.
Numerous commercial products are available to replace or supplement maternal colostrum. Most colostrum products are manufactured using bovine colostrum, whey, or bovine serum as sources of IgG. Products derived from bovine serum are preferable because they are most likely to result in the highest transfer of IgG to the calf. Commercial colostrum products are generally labeled as either colostrum supplements or colostrum replacements. Colostrum supplements generally have less than 100 g of IgG per dose and are meant to be used as a supplement to maternal colostrum. Given alone, colostrum supplements lack the IgG concentration necessary to prevent failure of passive transfer and they lack the necessary nutritional components to ensure calf survival and health. Colostrum supplements can be very useful to offer additional colostrum when the calf receives some maternal colostrum but concentration or volume offered by the dam is insufficient.
Colostrum replacements generally have greater than 100 g of IgG per dose and are meant to be used as a replacement when maternal colostrum is completely unavailable. Colostrum replacements are also formulated to supply the necessary nutrients required by the calf. Colostrum replacements are more expensive than colostrum supplements because they are more concentrated with antibodies and nutrients but may be worth the investment if you have to completely replace maternal colostrum. However, commercial colostrum replacers are never as good as fresh or frozen beef colostrum.
| Contributors | |||||
|---|---|---|---|---|---|
| Grant Dewell | Renée Dewell | Katy Lippolis | |||
Associate Professor |
Veterinary Specialist Center for Food Security/Public Health rdewell@iastate.edu 970-231-9654 |
||||
